When Dina’s* son was three, she had a gut feeling that something was wrong with her child’s behavior, but her pediatrician encouraged her to be patient and try different parenting techniques. When her child was four, he threatened to kill both his parents and himself.
At that point, Dina called the pediatrician in tears and asked, “What now?”

Dina’s son is among the five percent of children who are diagnosed as having a serious emotional disturbance (SED) in the United States. Behaviors of children with SEDs are characterized by severe symptoms that could range from suicidal ideation or attempt to harming others, setting fires, running away, destroying property, and exhibiting psychotic symptoms such as hallucinations or delusions.
Parents like Dina find themselves struggling to locate, navigate, and pay for the extensive services their children and family need. These services may include individual and family therapy, medication, respite care, classroom support, and inpatient hospitalization.
But in some severe cases, families reach a point where they cannot care for their child at home any longer. They have exhausted all of the available resources to help their child. Their child may become a danger to him or herself, to others, or might require extensive services that the family simply can no longer afford.
“There are no exact numbers, but anecdotal evidence suggests that some families with children with SEDs reach the devastating decision that the only remaining option is to consider placing their child in the foster care system,” says Monica Faulkner, co-director of the School of Social Work’s Child & Family Research Institute (CFRI).
“After exhausting all options, families begin to view relinquishment as one of the only ways to get their child’s mental health needs met. Other families face the reality that their child will likely be incarcerated.”
For the past five years, CFRI has been producing leading research on child and family wellbeing in Texas, with a strong emphasis on the child welfare system.
Recently, following a request from the Texas Department of Family and Protective Services, the CFRI research team explored the needs of families with children with SEDs and the resources available to them in the Lone Star State.
Led by Faulkner, associate director Beth Gerlach, and research coordinator Laura Marra, the goal of this study was to understand how systems could better meet the needs of families and prevent the relinquishment of children with SEDs. The study will inform recommendations to the 84th Texas Legislative session.
“Children’s mental health is a public health priority, not an issue for child protection,” Faulkner emphasizes. “We need to provide the necessary services to children with SEDs so families do not reach a point where relinquishment to foster care is an option.”
A predictable trajectory
Like other children, the behaviors and needs of each child with a SED are unique. Nevertheless, after interviewing service providers, families, and caregivers, the CFRI team found that parents of children with SEDs often follow a predictable help-seeking trajectory.
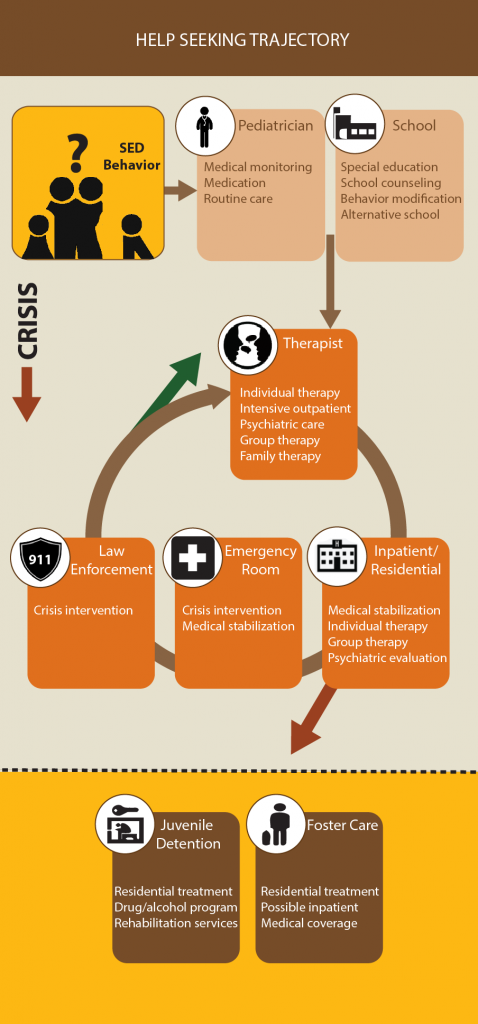 As was the case with Dina, this trajectory often starts as early as toddlerhood with a family taking their child to a pediatrician. The pediatrician may or may not recognize the early symptoms as requiring intervention. However, once the child enters school, teachers and school administrators express concern about the child’s behavior and functioning. Parents usually begin the complex process of advocating for school support and qualifying their child for special education services. They often seek additional help in the community from a therapist or child psychiatrist in order to obtain counseling services, diagnose mental illnesses, and receive medication management services for their child.
As was the case with Dina, this trajectory often starts as early as toddlerhood with a family taking their child to a pediatrician. The pediatrician may or may not recognize the early symptoms as requiring intervention. However, once the child enters school, teachers and school administrators express concern about the child’s behavior and functioning. Parents usually begin the complex process of advocating for school support and qualifying their child for special education services. They often seek additional help in the community from a therapist or child psychiatrist in order to obtain counseling services, diagnose mental illnesses, and receive medication management services for their child.
“With appropriate therapy, school supports and medication management, children can stabilize,” Gerlach says. “In fact, the parents we interviewed were able to recall a period of relative calm for the family, when there was a particular therapist who was able to develop a strong relationship with their child.”
If a strong therapeutic relationship does not develop, if the therapy is disrupted or if an event triggers the child’s behavior, the family often enters into a cycle of seeking emergency help. This cycle may include law enforcement, often called through 911 during violent episodes or episodes where self-harm is imminent. Law enforcement officers might arrest the child or transport him or her to an emergency room for psychiatric treatment.
Family members might also seek emergency assistance by taking the child directly to an emergency room, but emergency rooms are generally not equipped for psychiatric treatment. Once there, hospital staff might work to transfer the child to an inpatient psychiatric treatment facility—which in some cases may take days. While some families reported the benefits of inpatient care, services in psychiatric facilities vary greatly. The length of stay allowed is often too short, and families in the study felt that these facilities were not well regulated.
After leaving an inpatient facility, some parents described a brief “honeymoon” period when their child was able to reintegrate back into their family and utilize community-based therapy. Unfortunately, the cycle of law enforcement, emergency rooms, and inpatient facilities often becomes a norm for families. The research team found that many parents could not even recall the exact number of times they had been through the cycle described here.
“After moving through the emergency cycle multiple times, families are emotionally and financially exhausted,” Faulkner explains. “They might consider having their child enter the foster care system, or their child may enter the juvenile justice system. Either way, they are faced with a no-win situation, and a bond is broken between the parent and the child.”
Barriers to breaking the emergency cycle
“Timely access to quality mental health services is essential to help children with a SED stabilize and break the emergency cycle—or better, never go through it,” Marra states.
There are barriers to this timely access, however. Consistent with national data, the Texas families interviewed by the CFRI team cited cost as the primary reason why they were not able to access quality services for their children.
This might not be surprising in Texas, where an estimated 1 million children do not have health insurance, and less than 33% of doctors accept Medicaid.
Even with insurance, families in the study reported expensive co-pays, such as $400 a month for medication or $8,000 for just one child’s inpatient stay. Caregivers also pointed out that insurance companies, instead of the child’s needs, determine the type and length of available services.
“While mental health services costs are high for both families and taxpayers, let’s remember that the costs of untreated mental health illnesses are even higher,” Gerlach says. “The National Mental Health Association estimates that untreated mental illness costs $105 billion in lost productivity each year as well as $8 billion in crime and welfare expenditures.”
Even when families have the financial resources, they are likely to experience long waits, particularly for child psychiatrists. Interviewed caregivers reported waits as long as two years for an assessment. Delays in evaluation, treatment and intervention result in a progression of the mental health condition, and create a cycle of insufficient available treatment: by the time the child is able to access a service, he or she is often already in need of the next level of service.
Where to Start
Caregivers reported “wraparound,” a delivery model for services that focus on the holistic needs of the child and the family, as incredibly useful. Services under wraparound go beyond therapy and medication to include non traditional services such as respite care, support groups, transportation, employment services, and home modifications. Most parents could also speak of one or two specific therapies, including specialized music or art therapy, that were of great help to their child.
Communities and schools were identified as the most accessible places for parents to obtain these useful mental health services for their children. Even with co-pays, counselors in the community cost families less than inpatient treatment.
A very promising initiative is Youth Empowerment Services, or the YES program, which parents in the study most frequently identified as a needed service. This program started in Texas in 2012, in response to concerns about parents relinquishing custody of children with SEDs to foster care after having exhausted all their resources.
The YES program uses Medicaid funds to increases community–based services and avoid expensive inpatient psychiatric hospitalizations. Eligibility does not consider parental income, and thus removes the need for parents to relinquish their child to foster care in order to access Medicaid-covered treatments.
“The bottom line is that children’s mental health is a public health priority and it is everyone’s responsibility,” Faulkner says. “The purpose of our child welfare system is to serve children who have been maltreated. It is not designed, nor should it be designed, to provide mental health treatment to all Texas’ children. Rather, Texas communities have to step up and help families and children get the support they need.”
*Names have been changed
By Andrea Campetella
